What is In Vitro Fertilization or IVF?
If you’re facing difficulties with fertility, your doctor might initially recommend surgery, artificial insemination and specific medications as a preliminary measure before exploring other treatment options. However, if these methods prove ineffective, the utilization of Assisted Reproductive Technology (ART) methods may be considered to address your infertility.
ART encompassed a range of medical procedures primarily designed to treat infertility. This technology involves several techniques, including Intrauterine Insemination (IUI), Intracytoplasmic Sperm Injection (ICS), In Vitro Maturation (IVM), and the widely used In Vitro Fertilization (IVF), which is commonly prescribed method for couples based on the underlying cause of their infertility.
The term "in vitro" originates from Latin and translates to "in beaker" or "in glass." This designation stems from the fact that the procedure occurs outside the human body, typically in a controlled laboratory environment. In simpler terms, IVF involves the fertilization of a woman's eggs with sperm in a laboratory, followed by the transfer of these fertilized eggs, known as embryos, into the woman's uterus to facilitate their growth.
In other words, following several phases of cell division, doctors transfer one or more egg cells into the uterus. On the fifth day, an eight-cell embryo is carefully placed in the uterus, allowing the natural progression of embryonic development. This process begins with ovulation induction in women, followed by the collection and development of an appropriate number of eggs in the laboratory. Once the eggs have matured, they are fertilized using sperm. After assessing the quality of egg cells, one or more embryos are transferred to the mother’s uterus.
The Evolution of In Vitro Fertilization in Iran
The progress of IVF treatment in Iran has been shaped by the collaborative efforts of IVF pioneers and a multidisciplinary team of experts, supported by the endorsement and enthusiastic backing of Shia jurists.
This synergy has led to significant milestones in assisted reproductive technologies. Notably, Iran achieved remarkable breakthroughs, including the first successful pregnancy through retrograde ejaculation using intrauterine insemination in 1992, the first baby born from intracytoplasmic sperm injection and egg donation in 1994, and the first baby conceived through ICSI in Iran and percutaneous epididymal sperm aspiration in 1996-1997.
Subsequently, in 1998, Iran accomplished another milestone by transferring the first embryo derived from testicular spermatozoon via microinjection, followed by the first successful birth following pre-implantation genetic diagnosis (PGD) in 2004.
Today, the utilization of IVF has become widespread in Iran, serving various purposes such as preimplantation genetic screening (PGS) for genetic disease prevention, preimplantation genetic diagnosis (PGD) for sex selection, as well as facilitating sperm, egg, and embryo donation, surrogacy, fertility preservation, and fertility conservation through methods like cryopreservation (freezing) of eggs, sperm, and embryos. This comprehensive range of reproductive services demonstrates Iran's commitment to advancing and expanding the possibilities of assisted reproductive technologies.
Is the Practice of IVF Allowed in Iran?

Iran has established numerous fertility treatment centers that offer a range of infertility treatments, including IVF, IUI, ICSI, egg donation, sperm donation, surrogacy, PGS (genetic screening), and PGD (sex selection), all of which are conducted in accordance with the country's regulated laws. IVF is legally permitted in Iran as it serves as a necessary procedure for various infertility treatments. By legalizing the use of Assisted Reproductive Technologies (ART), Iran has made significant advancements in the field of infertility treatment, positioning itself as a leading country in the region, particularly for Muslim patients, alongside European and American counterparts.
Within Islam, varying perspectives exist regarding the utilization of assisted reproductive technologies. The Sunni branch tends to impose more restrictions compared to Shia schools. However, both branches of Islam permit the use of in vitro fertilization for couples who use their own gametes for insemination. In 1999, Ayatollah Khamenei, the Supreme Leader of Iran, granted approval for the use of donor eggs, sperm, and embryos under specific conditions, thus further addressing the ethical considerations within the Islamic context.
Why Choose IVF Treatment in Iran?

When considering IVF treatment abroad, there are compelling reasons to choose Iran as the destination. Iran offers numerous advantages that have made it a popular choice for couples seeking IVF treatment. These advantages include:
•Affordability and Cost-effectiveness:
IVF treatment in Iran is significantly more affordable compared to many other countries, making it a cost-effective option for couples seeking fertility treatment.
•Utilization of Donor Eggs and Sperm:
Iran allows the use of donor eggs and sperm, providing additional options for couples with specific fertility issues. This increases the chances of success for those facing challenges in conceiving with their own gametes.
•Impressive Success Rates:
Iran has achieved impressive success rates in IVF treatment, with some clinics reporting success rates as high as 70%. This demonstrates the effectiveness and reliability of IVF procedures in the country.
•Respect for Cultural Considerations:
Iran has strict regulations and ethical guidelines governing IVF treatment, ensuring that patients' cultural and ethical concerns are respected and addressed throughout the process.
•Experienced and Skilled Medical Professionals:
Iranian IVF specialists have extensive experience and expertise in the field. They have undergone rigorous training and are skilled in performing successful IVF procedures.
•Cutting-Edge Technological Advancements:
Iranian clinics are equipped with state-of-the-art technology and modern facilities, ensuring that patients receive the highest standard of care during their IVF treatment.
•Availability of Surrogate Mothers:
In Iran, the availability of surrogate mothers is legally regulated. This offers a viable solution for couples who require the assistance of a surrogate to carry and deliver their embryos, enhancing the chances of a successful outcome.
Beyond the medical benefits, choosing Iran as a medical destination offers the added opportunity to experience the rich cultural heritage and diverse landscapes of the country. From breathtaking natural wonders to ancient ruins, bustling cities to vibrant traditions, Iran provides a captivating and unforgettable travel experience for visitors.
Cost of IVF Treatment in Iran
The cost of IVF procedures can differ significantly based on various factors on a global scale, and for many couples, it can be financially burdensome, especially considering that most medical insurance plans do not cover IVF.
However, the cost of IVF in Iran typically ranges between $3,000 and $5,000 per cycle, which includes all routine procedures, tests, medications, and treatments. This makes IVF in Iran much more affordable compared to many other countries. The high quality of fertility treatment services in Iran, coupled with reasonable fees charged by specialists and clinics, has attracted many couples from abroad.
In contrast, the cost of IVF in countries like the United States can be as high as $15,000 per cycle, not including medication expenses. The average cost in the United Kingdom ranges from $5,000 to $7,000 per cycle, while in Mexico, it averages around $6,500. On the other hand, India offers at an average cost of $4,000, and in Turkey, it amounts to approximately $3,700.
The reason behind the low price of IVF in Iran in comparison with other countries is due to factors such as lower doctor’s wages and the affordability of clinic services. The comprehensive cost typically covers consultations, medications, surgical and diagnostic procedures, as well as post-op care specialized services like pre-implantation genetic diagnosis (PGD). Some couples may also require additional services like egg donation, which can increase the overall cost of treatment.
With the relatively low cost of IVF in Iran and its reputation for providing high-quality care, many patients choose to travel there for treatment. The affordable pricing, along with the availability of complementary techniques like PGD and microsorting for sex selection, makes IVF in Iran an attractive option for couples seeking fertility assistance.
The expenses associated with sex selection can differ depending on the country and specific clinic. In Iran, the average price for PGD is approximately $1,000, while the cost for Microsorting is around $700. It's important to note that these charges are supplementary and are added to the overall cost of IVF treatment.
Overall, although the IVF cost varies worldwide, yet Iran stands out as a cost-effective choice, offering competitive pricing without compromising on the quality of care provided.
Can IVF in Iran Be Recommended for Everyone?

Not every couple will receive a prescription for IVF in Iran, as it is primarily recommended for individuals who experience specific conditions as described below:
•Women under the age of 43 are generally considered good candidates for IVF in Iran. Younger age is associated with better chances of success.
•Leading a healthy lifestyle, including factors such as maintaining a balanced diet, regular exercise, and avoiding harmful habits like smoking and excessive alcohol consumption, can contribute to better outcomes.
•Significant ovarian dysfunction, such as polycystic ovary syndrome (PCOS).
•Issues with antibodies that harm sperm or eggs.
•Genetic disorders that contribute to recurrent miscarriages or the risk of passing on genetic conditions to the child. By testing embryos, it is possible to select those without genetic abnormalities.
•Endometriosis, characterized by the abnormal growth of uterine tissue inside or outside the uterine cavity, which does not respond to medical interventions or surgery. This condition impairs the functioning of the ovaries and fallopian tubes.
•Couples who have previously undergone unsuccessful infertility treatments like intrauterine insemination (IUI).
•If a patient is preparing to undergo cancer treatment, it is possible to preserve her eggs by freezing them at specialized fertility centers until a suitable time for pregnancy.
•Obstruction, absence or damage of one or both fallopian tubes in women that cannot be resolved through surgery, preventing the embryo from reaching the uterus or the egg from being fertilized
•Infertility related to male factors, such as low sperm count or sperm motility, as well as abnormal sperm morphology.
•Leiomyoma, also known as uterine fibroids, refers to noncancerous tumors made of smooth muscle cells in the uterine wall. These growths can interfere with the implantation of fertilized eggs and are commonly observed in women in their 30s and 40s. If a patient has previously undergone fallopian tube removal or sterilization procedures (for instance, tubal ligation), options such as tubal ligation reversal surgery or IVF may be recommended to achieve pregnancy.
•Difficulties with ovulation, ovarian failure and diminished ovarian reserve in females due to the reasons like premature menopause or medical conditions like cancer.
•Unexplained fertility problems with no identifiable cause that result in infertility.
As mentioned earlier, not everyone is an ideal candidate for IVF. Patients with fibroid tumors, high blood pressure, ovarian dysfunction, hormonal imbalances, and uterine irregularities may have lower chances of success with IVF.
What Procedures are Needed Before IVF in Iran?
Before undergoing an IVF treatment in Iran, your doctor will ask for a more detailed assessment and a number of tests, using your and your partner’s eggs/sperm cells. These assessments include:
•Sonography:
Sonography or ultrasound is performed during the second or third day of the mother’s menstrual cycle to assess the conditions of the ovaries and uterus. This diagnostic procedure is essential for evaluating the health and status of these reproductive organs.
•Ovarian Reserve Assessment:
This evaluation involves determining the quantity and quality of a woman’s remaining egg supply, which can be valuable in predicting the response to ovulation-including drugs and informing the treatment plan. To assess this, your doctor may examine levels of follicle-stimulating hormone (FSH), estradiol (estrogen), and anti-molybdenum hormone in your blood during the early days of your menstrual cycle. These tests, along with an ultrasound of your ovaries, provide insights into the quantity and quality of your eggs. The results help determine whether your ovaries are likely to respond to fertility medication or if further screening is necessary.
•Sperm Analysis:
Evaluating and analyzing the characteristics and overall health of sperm is an essential step in the IVF treatment process. Your doctor will conduct a semen analysis shortly before initiating the IVF cycle to examine factors such as sperm count, motility (movement), and morphology (shape). To ensure the accuracy of the results, it is recommended to perform the analysis close to the start of the treatment. Based on the findings, the doctor will determine whether conventional IVF or intracytoplasmic sperm injection (ICSI) is the most valuable method for fertilizing the eggs.
•Infectious Disease Screening:
Conducting tests to identify the existence of communicable diseases is a crucial step in the process. Both you and your partner will undergo screening for infectious illnesses, including HIV. This comprehensive test covers a range of infectious and viral diseases in both men and women, prioritizing the well-being of medical staff and laboratory personnel. Additionally, this screening procedure plays a vital role in safeguarding the IVF embryos from potential infections.
•Experimental Embryo Transfer:
Implementing a procedure to transfer embryos under carefully controlled experimental conditions is the next step in the process. This procedure helps in selecting the most suitable method for embryo transfer and identifying women who may encounter challenges during this process. To ensure optimal results, your physician may conduct a simulated embryo transfer to assess the depth of the uterine cavity and determine the technique that is most likely to successfully implant the embryo in your uterus. This allows for a more informed and personalized approach to the embryo transfer process.
•Uterine Cavity Imaging:
Employing diagnostic techniques to visualize and evaluate the interior of the uterus is the last part of this process. Uterine imaging is conducted to ensure the uterus is prepared for successful embryo implantation shortly after commencing the treatment cycle. This method helps identify any potential disorders or adverse conditions that may affect pregnancy outcomes. Before initiating the IVF procedure, your doctor will examine the uterine lining using various approaches. This may involve Sonohysterography, a procedure where fluid is gently introduced into the uterus through the cervix, allowing for detailed ultrasound imaging of the uterine cavity. Additionally, hysteroscopy may be employed, which entails inserting a slender, flexible, and illuminated telescope called a hysteroscope through the vagina and cervix to directly visualize the uterus.
The Process of IVF Treatment in Iran
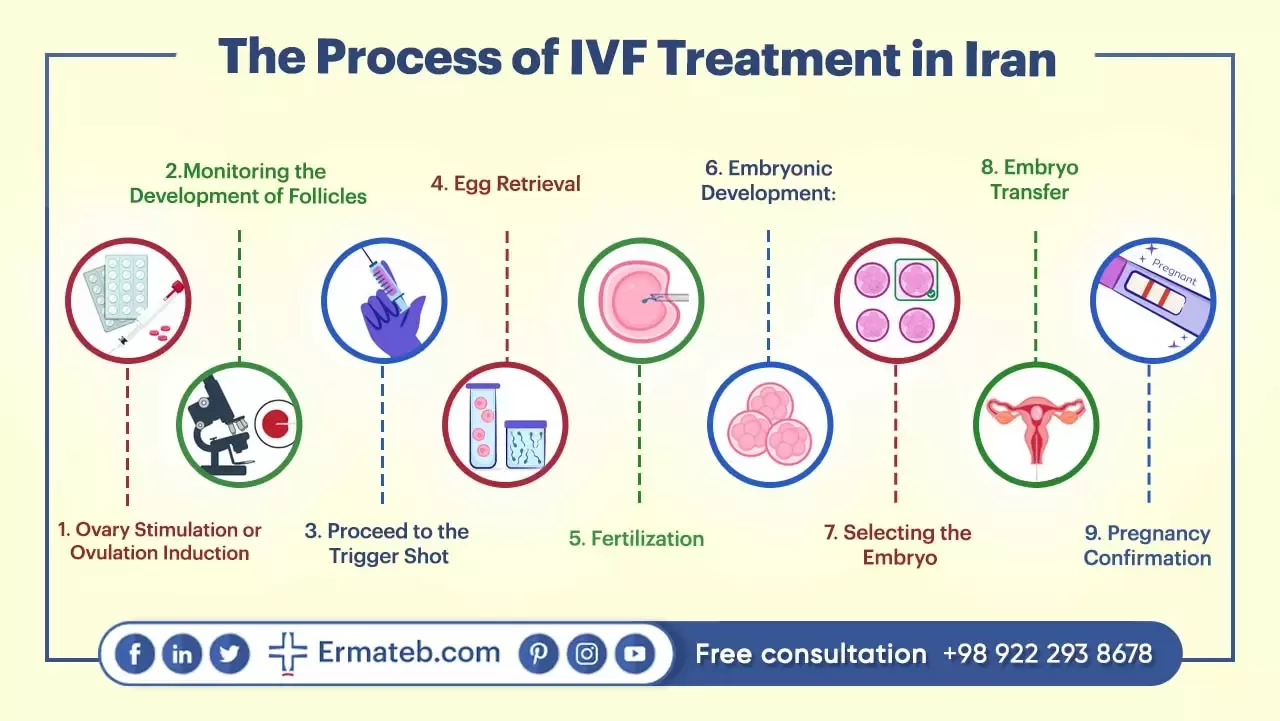
The IVF treatment process in Iran consists of several essential steps that ultimately lead to pregnancy. These steps are outlined as follows:
1. Ovary Stimulation or Ovulation Induction
The IVF cycle commences with the administration of synthetic hormones to stimulate the ovaries to produce multiple eggs, surpassing the usual monthly development of a single egg. Generating multiple eggs is necessary as not all eggs fertilize or develop normally.
Various medications are utilized for this purpose, and your doctor will collaborate with you to determine the most appropriate medications and their timing. These medications include:
Ovarian Stimulation Drugs:
These injections contain follicle-stimulating hormone (FSH), luteinizing hormone (LH), or a combination of both to stimulate the ovaries and promote the development of multiple eggs.
Oocyte Maturation Medications:
Once the follicles are ready for egg retrieval, typically after 8 to 14 days, medications like human chorionic gonadotropin (HCG) or others are used to aid in the maturation of the eggs.
Medications to Prevent Premature Ovulation:
These medications, such as leuprolide or sterolix, prevent the body from prematurely releasing developing eggs.
Medications to Prepare the Uterus Lining:
Prior to egg retrieval or embryo transfer, your doctor may recommend progesterone supplements to enhance the receptivity of the uterine lining for implantation.
2. Monitoring the Development of Follicles
Typically, one to two weeks of ovarian stimulation and follicle development is required before the eggs are ready for retrieval.
Monitoring the growth of follicles, which are fluid-filled sacs in the ovaries where eggs mature, is accomplished through vaginal ultrasound imaging. This imaging test allows for tracking the progress of follicles.
Additionally, blood tests are conducted to measure your response to the ovarian stimulation drugs. Estrogen levels usually increase as follicles develop, while progesterone levels remain low until after ovulation.
3. Proceed to the Trigger Shot
The trigger shot is administered once your follicles have reached the desired state of readiness. This injection aids in the full maturation of your eggs, preparing them for fertilization. Approximately 36 hours after receiving the trigger shot, you will visit the clinic for the retrieval of your eggs.
4. Egg Retrieval
Approximately 34 to 36 hours following the final injection and before ovulation, the ovulation procedure can be conducted at the doctor's office or clinic.
-During the process of egg retrieval, you will receive sedatives and painkillers to ensure your comfort.
-The standard method for recovery is transvaginal ultrasound aspiration. This involves the insertion of an ultrasound probe into the vagina to locate the follicles. Subsequently, a thin needle is guided through the vagina using the ultrasound as a reference, reaching the follicles to retrieve the eggs.
-If transvaginal ultrasound access is not feasible, an abdominal ultrasound may be employed to guide the needle during the retrieval process.
-Using a needle connected to a suction device, the eggs are carefully removed from the follicles. This process usually takes around 20 minutes to extract a few eggs.
-Following egg retrieval, you may experience cramping, as well as a sensation of fullness or pressure.
-The mature eggs are then placed in a nutrient-rich solution called the culture medium, where they are incubated. Healthy and mature eggs will be mixed with sperm to facilitate embryo creation. However, it's important to note that not all eggs may be successfully fertilized.
In certain cases, IVF cycles may require cancellation before egg retrieval due to multiple reasons. If your cycle is cancelled, your doctor may recommend adjustments in medication or dosage to enhance the response in future IVF cycles. Alternatively, you may be advised to consider using an egg donor for future attempts. The reasons for cancellation can include:
Insufficient development of follicles:
When an inadequate number of follicles are developing, it may be necessary to cancel the cycle.
Premature ovulation:
If ovulation occurs before the scheduled retrieval, the cycle may be cancelled.
Excessive follicle growth and risk of ovarian hyperstimulation syndrome:
When the follicles overgrow, it poses a risk of ovarian hyperstimulation syndrome, leading to the cancellation of the cycle.
Other medical concerns:
Various medical issues or complications may arise that necessitate the cancellation of the IVF cycle.
5. Fertilization
At this stage, an embryologist, who is a specialist in sperm, eggs, and embryos, will examine your eggs at first and then, proceeds to the fertilization. There are two commonly employed methods for fertilization:
-Conventional Insemination: In this approach, mature eggs and healthy sperm are combined and incubated overnight.
-Intracytoplasmic Sperm Injection (ICSI): With ICSI, a single healthy sperm is directly injected into each mature egg. This method is typically used when there are concerns about the quality or quantity of semen, or if previous IVF cycles have not resulted in successful fertilization.
In certain situations, the doctor may suggest alternative fertilization techniques prior to embryo transfer.
Assisted Hatching:
Around five to six days after fertilization, an embryo naturally emerges from its protective membrane (zona pellucida) to facilitate implantation in the uterine lining. However, in cases of advanced maternal age or multiple unsuccessful IVF attempts, your doctor may recommend assisted hatching. This procedure involves creating a small opening in the zona pellucida shortly before transfer, facilitating the embryo's emergence and implantation. Assisted hatching is also beneficial for frozen eggs or embryos as it helps to harden the zona pellucida.
Pre-implantation Genetic Testing:
As embryos develop in the incubator, they reach a stage where a small sample can be extracted and tested for specific genetic disorders or the correct number of chromosomes. This testing typically takes place after 5 to 6 days of development. Embryos that do not exhibit genetic abnormalities or chromosomal issues can be selected for transfer to the uterus. While pre-implantation genetic testing reduces the risk of transmitting certain genetic conditions, it cannot completely eliminate it. Prenatal testing may still be recommended to ensure a comprehensive assessment.
Egg Donation:
If your eggs are deemed unsuitable for fertilization, considering egg donation may be an option. This involves using donor eggs from a third party, whether anonymous or known., to produce embryos that can be implanted into your uterus for pregnancy.
In Vitro Maturation (IVM):
For certain women who are unable to naturally produce mature eggs, an alternative approach called In Vitro maturation (IVM) is utilized to retrieve and artificially mature immature eggs outside the body.
6.Embryonic Development:
Following successful fertilization, the eggs undergo a remarkable transformation during the IVF process. Within approximately three days, some of the fertilized eggs develop into embryos consist of six to ten cells.
As the progress continues, by the fifth day, a subset of these embryos further advances into blastocysts. These blastocysts are characterized by a fluid-filled cavity and differentiated tissues that will eventually from both the baby and the placenta.
During this critical stage of development, embryologists closely monitor the embryos' growth and progression. The blastocysts are carefully assessed for their quality and viability, considering factors such as the number and arrangement of cells, the presence of a well-defined inner cell mass, and the expansion and integrity of the fluid-filled cavity.
It is important to note that not all embryos will reach the blastocyst stage, and their development can vary. The expertise of the embryology team and their rigorous evaluation ensure that the embryos selected for transfer or cryopreservation have the highest potential for successful implantation and healthy pregnancy.
7.Selecting the Embryo:
At the stage of selecting the embryo, the most promising embryos are identified for transfer into the uterus, maximizing the chances of a successful pregnancy.
In some cases, excess embryos of high quality may be cryopreserved for future use, offering the possibility of additional attempts without the need for repeated ovarian stimulation and egg retrieval.
8.Embryo Transfer:
The next crucial stage in the IVF process is the embryo transfer, which typically occurs at your doctor’s office or a specialized clinic. This procedure is typically scheduled withing two to five days following egg retrieval.
To ensure your comfort during the process, you may be given a mild sedative. It is worth noting that the procedure itself is usually painless, though you may experience mild cramping.
During the embryo transfer, a skilled doctor will delicately insert a long, thin, and flexible tube known as a catheter into your vagina, passing it through the cervix and into the uterus. At the end of the catheter, a syringe containing one or more embryos suspended in a small amount of fluid will be attached.
With precision and expertise, the doctor will utilize the syringe to gently place the embryo or embryos into your uterus. This step aims to maximize the chances of successful implantation and subsequent pregnancy.
Following the transfer, the embryo undergoes a crucial period of development. If everything goes according to plan, the embryo will implant into the lining of your uterus around six to ten days the egg retrieval stage. Successful implantation is a crucial milestone on the path to healthy pregnancy.
It’s important to note that the number of embryos transferred may vary depending on several factors, including your age, previous IVF outcomes, and specific medical considerations. The decision regarding the number of embryos to transfer is typically made in consultation with your doctor, taking into account factors such as the quality and developmental stage of the embryos.
During the subsequent days and weeks after the transfer, close monitoring and potential hormone supplementation may be provided to support the implantation process and optimize the chanced of a successful pregnancy. Regular follow-up appointments and pregnancy tests will be scheduled to track your progress and confirm the success of the procedure.
9.Pregnancy Confirmation
Once the embryo has successfully implanted in the uterus, it has the potential to develop into a healthy baby. In cases where multiple embryos are transferred, the likelihood of achieving a pregnancy increases, along with the possibility of a multiple pregnancy.
Consequently, it is not uncommon for approximately 20% of babies conceived through in vitro fertilization to be twins, triplets, or even higher-order multiples.
Approximately two weeks following the embryo transfer, you can take a pregnancy test to determine if implantation has occurred. This test serves as an initial indicator of pregnancy. However, it’s important to not that a positive result on the pregnancy test does not guarantee a successful and ongoing pregnancy. Further monitoring and assessments will be conducted to confirm the viability and progress of the pregnancy.
How Long Does IVF Process Take in Iran?
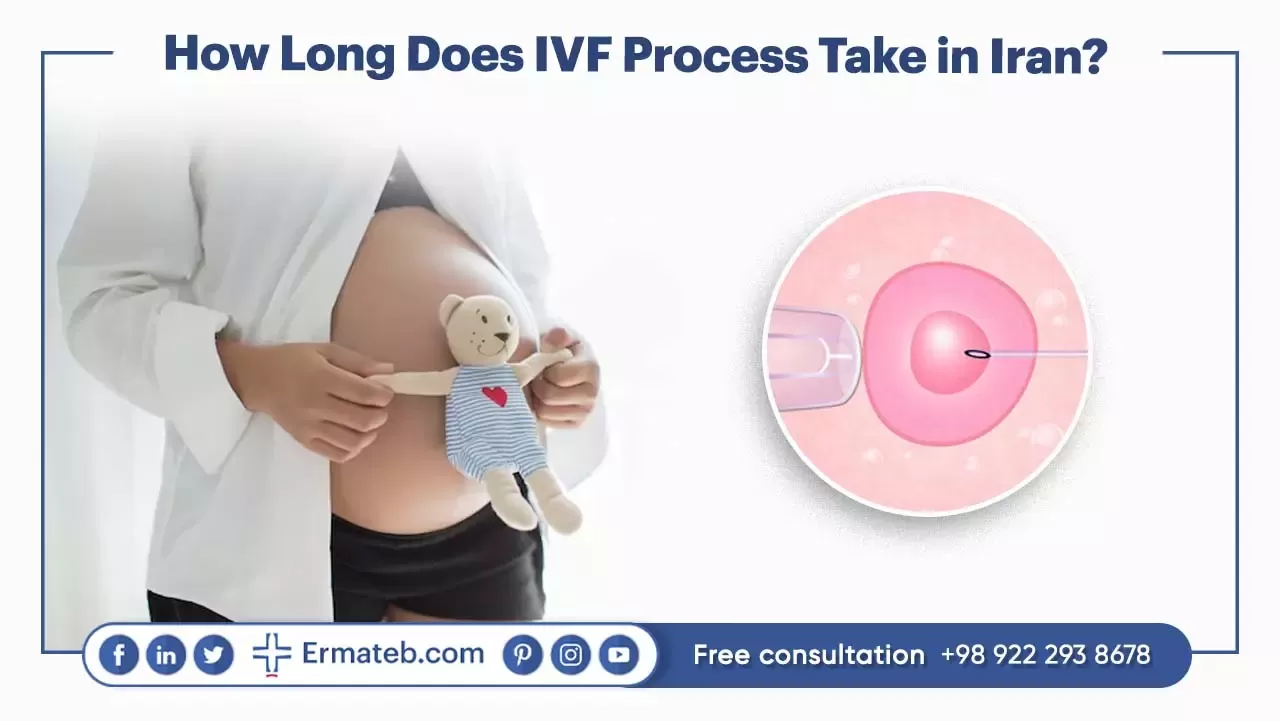
A complete cycle of IVF treatment in Iran typically lasts between 6 to 8 weeks. The process begins with pre-operative procedures, including general and hormonal tests, uterine and ovaries ultrasounds, viral lab tests, and sperm and semen analysis. Once the woman’s menstruation cycle starts, prescribed medication is provided with the dosage determined based on factors such as age, weight, and height.
Following egg retrieval and sperm collection, the embryos are developed in a laboratory setting. On day 17 or 18 of the cycle, the embryo(s) are transferred to the woman’s uterus. Two weeks later, a blood test is conducted to determine the success of the pregnancy.
Recovery time after the procedure in Iran can also differ from person to person, similar to recovery after any major surgery. Patients should expect to spend some time recovering in the ward before being discharged. The immediate recovery period can be influenced by factors such as the type of sedation used and its duration.
Causes of IVF Treatment Failure

The success of IVF treatment hingers upon the successful completion of each stage, Consequently, if any stage encounters difficulties or setbacks, the overall IVF outcome may be affected. Several factors can contribute to the failure of IVF, including:
-Poor Ovarian Response:
In some cases, the ovaries may not adequately respond to the medications used during the initial stages of IVF. This can result in a lower number or poor quality of eggs retrieved, decreasing the chanced of successful fertilization and implantation.
-Suboptimal Egg and Sperm Quality:
The quality of both the eggs and sperm plays a crucial role in the success of IVF. If the retrieved eggs or sperm exhibit poor quality, it can impede successful fertilization or hinder the development of healthy embryos.
-Genetic Abnormalities:
Genetic issues within the formed embryos can contribute to IVF failure. These abnormalities can affect embryo development and reduce the chanced of successful implantation and pregnancy.
-Uterine Disorders:
Certain uterine conditions or disorders can hinder the implantation of embryos, leading to IVF failure. Uterine abnormalities or complications, such as fibroids or polyps, may interfere with the embryo’s ability to attach to the uterine lining.
-Female Age:
As woman age, both the quantity and quality of their eggs decline. This decline significantly affects the likelihood of achieving a clinical pregnancy or live birth following IVF treatment. Women under the age of 35 generally have the highest chanced of success in IVF procedures dur to better egg quality and quantity.
-Embryo Quality:
During IVF, the eggs and sperm are combined in a laboratory setting to create embryos. While embryos may appear healthy in the lab, there is a possibility that they may not successfully implant into the uterus due to undetectable flaws. IVF laboratories evaluate the quality of embryos using a scoring system, selecting the best ones for transfer back into the uterus.
-Implantation Issues:
Failure of embryos to successfully implant in the uterus can be attributed to various factors. These may include the presence of uterine polyps, and early rise in progesterone levels, a thin endometrial lining, or uterine infection.
-Lifestyle:
Maintaining a healthy lifestyle before and during IVF can positively impact the chances of conception, similar to natural pregnancies. It is advisable to cease smoking several months prior to commencing IVF, as smoking has been linked to reduces fertility.
-Chromosomal Abnormalities:
Chromosome abnormalities in embryos can lead to IVF failure. These abnormalities occur when there is a missing, extra, or irregular arrangement of chromosomal DNA in the embryo. The body may reject embryos with chromosomal anomalies, which can occur during early embryonic development or be inherited from the parents.
-Egg Abnormalities:
The structure of the human egg is complicated, making it sensitive to damage that renders it nonviable. With age, the spindle apparatus responsible for proper chromosomal distribution weakness, increasing the likelihood of abnormal chromosome distribution in the embryo.
-Abnormal Sperm:
While less frequent than other factors, abnormal sperm can still impact the success of an IVF cycle. Sperm mobility is crucial for fertilization, as the tail propels the sperm from the female reproductive system towards the egg. Studies have shown that chromosomal abnormalities are more prevalent in sperm that in eggs.
In the event of IVF failure, couples have the option to undergo the process again after a period approximately 2 or 3 menstrual cycles. This delay allows the woman’s body to return to its normal menstrual cycle and provides time for physical and emotional recovery. By repeating the IVF process, couples have another opportunity to achieve a successful pregnancy.
The Side Effects of IVF Treatment
While fertility drugs used in IVF treatment have been established as safe, it is important to be aware of potential side effects that may arise from these medications. Each woman's response to hormone-based drugs can vary, resulting in different experiences. Some common side effects include:
•Abdominal Distention
•Discomfort or Tension in the Stomach Area
•Sensitivity or Soreness in the Breasts
•Experiencing Dizziness and Weakness
•Having Sickness or Nausea
•Emotional Fluctuations
•Cranial Discomfort
•Bruising at the Injection Site
•Adverse Reactions to Medications
•Light Vaginal Bleeding
•Risk of Infection
IVF Success Rates in Iran
The success of an IVF procedure in Iran is determined by various factors, and it is important to understand the implications associated with age and lifestyle choices. After two weeks of undergoing IVF, a positive pregnancy test indicates a successful process.
Research suggests that women under the age of 35 have a higher chance of achieving pregnancy, with rates exceeding 40%. However, as a woman's age increases, the likelihood of pregnancy decreases. The success rates are often reported based on age, reflecting the downward trend in IVF success as women get older. The success rates per age category are as follows:
-Under the age of 35: Approximately 47% success rate.
-Ages 35 to 37: Around 40% success rate.
-Ages 38 to 40: Approximately 27% success rate.
-Over the age of 40: A modest success rate of about 7%.
While age plays a significant role, the couple's lifestyle choices also impact IVF outcomes. Smoking and leading a stressful lifestyle are known to have negative effects. It is crucial to consider these factors in conjunction with age when assessing the chances of success.
Choosing the right medical center or clinic is a critical factor in determining the success rate of IVF. Skilled doctors in Iran can provide valuable support throughout the entire procedure. However, the success rate depends on several other factors as well. Maternal age, embryo quality, sperm quality, uterus lining, general health, and lifestyle choices all play a role in determining success.
According to data from the US Centers for Disease Control and Prevention (CDC) in 2018, the average success rates for IVF, considering both fresh and frozen embryo transfer, were as follows:
-Women under the age of 35: 6% success rate.
-Women aged 35 to 37: 5% success rate.
-Women aged 38 to 40: 9% success rate.
-Women over the age of 40: 5% success rate.
It is important to note that IVF success rates are not comprehensive indicators and should be assessed in conjunction with individual factors that may impact the treatment's outcome. Consultation with medical professionals and considering the specific circumstances of each patient is crucial for determining the likelihood of success in an IVF treatment.
Can I Select the Gender of the Embryo in the IVF Treatment in Iran?
In Iran, fertility centers and hospitals offer artificial sex selection through different techniques. However, it is generally recommended for couples who already have children and seek family balancing by having another child.
Sex selection, also known as gender selection, is a procedure offered in IVF to help couples conceive a baby of their preferred sex. Fertility clinics often provide this option to IVF candidates, but it is important to note that thorough consultations are conducted to consider various factors before proceeding with the treatment.
There are two main techniques for sex selection in IVF: Microsorting and Pre-implantation Genetic Diagnosis (PGD).
•Microsorting:
Microsorting is a sperm sorting procedure that can be used in both IVF and IUI. This technique involves sorting individual sperm using a laser flow cytometer to separate X and Y chromosome-bearing sperm. Microsorting has a higher success rate for conceiving girls (around 90%) compared to boys (75%).
•Pre-implantation Genetic Diagnosis (PGD):
PGD involves the selection of high-quality embryos through genetic testing is an IVF cycle. This procedure actually includes a comprehensive screening process before embryo transfer, including essential examinations and tests to determine the gender of the fetus. While the primary aim of PGD is to prevent genetic disorders in IVF babies, it can also be used to determine the baby’s sex, allowing parents to choose the desired gender for the embryo. During the IVF and ICSI procedures, an intriguing possibility arises—the ability to predict the fetus's sex before transferring it to the uterus using the PGD technique.
After the formation of embryos in the IVF process, a specific cell is isolated from the developing embryo for thorough genetic and chromosomal analysis. This technique enables accurate identification of the embryos' sexes, allowing the selection of an embryo with the desired gender for transfer to the mother's uterus.
The success rate of PGD is nearly 100%, ensuring that if the IVF is successful, the baby will be of the predetermined sex.
These advancements in IVF, along with techniques like PGD, provide prospective parents with greater control over their reproductive journey. They grant the ability to choose embryos that align with their preferences and aspirations for their family, offering an unprecedented level of choice in the conception process.
Best IVF Centers in Iran
Iran is renowned for its numerous well-equipped IVF centers and highly skilled IVF surgeons, making it a sought-after destination for both local residents and international patients seeking infertility services. These leading fertility centers in Iran excel in the field of assisted reproductive technology, boasting state-of-the-art equipment and experienced experts.
These clinics have gained a reputation for their exceptional success rates and proficiency in providing a wide range of services, including gamete donation, IVF, ICSI, and surrogacy. They are committed to implementing the latest methodologies and advanced technologies, ensuring the highest chances of patient success.
The dedicated team of experts at these clinics offers compassionate and diligent care, guiding patients through their journey to parenthood. The clinics prioritize the well-being of their patients, providing a private and comfortable environment that supports both their physical and emotional needs. With sophisticated diagnostic tools and personalized treatment plans, these clinics strive to achieve the best possible pregnancy outcomes.
When seeking the best IVF clinic, it is essential to consider factors such as experienced and qualified medical staff, comprehensive assisted reproductive technology (ART) facilities, high success rates, personalized treatment plans, supportive care, and transparent policies.
By choosing Ermateb, each patient will be carefully referred to the most suitable center based on their specific needs and arrival time, ensuring they receive the highest quality care available.


 Arabic
Arabic
 German
German
 Persian (Farsi)
Persian (Farsi)
 Russian
Russian
 Beauty
Beauty


 Medical
Medical





 Hotels
Hotels
 Hospitals
Hospitals































![Frequently asked question about [name]](/v2tem/images/pages/service/faq-image.webp)
